The global healthcare fraud analytics market was valued at USD 1.73 billion in 2021 and it is predicted to surpass around USD 11.4 billion by 2030 with a CAGR of 23.31% from 2022 to 2030.
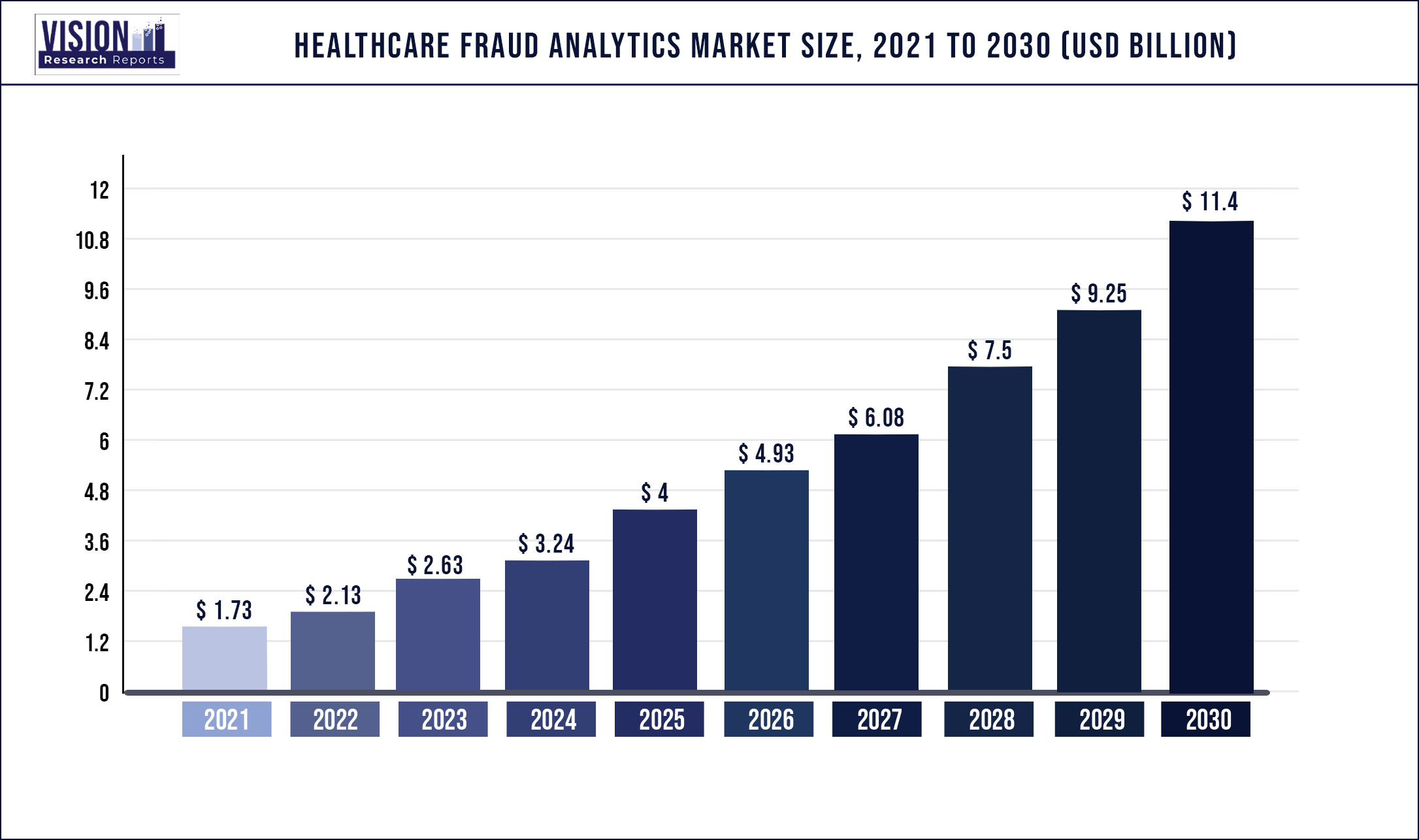
The rising incidence of fraudulent activities in the healthcare sector, increasing number of patients seeking health insurance, high returns on investment, and the increasing number of pharmacy claims-related frauds are the major drivers propelling the market growth.
The COVID-19 pandemic has drastically affected the healthcare industry. The healthcare industry has observed various fraud cases on the part of doctors, patients, physicians, and other healthcare specialists. It is observed that many medical specialists and healthcare providers are engaged in fraudulent activities for profit gains. Many instances prove the increasing number of fraud cases during the COVID-19 pandemic.
The adoption of software used for fraud detection by insurance companies is increasing due to the rising availability of the same in developed regions. For instance, in February 2022, The Canadian Life and Health Insurance Association (CLHIA) launched an industry initiative to pool claims data and use advanced artificial intelligence tools which enhance the investigation and detection of benefits fraud.
Moreover, in June 2021, Artivatic launched the Alfred- AI Health Claims platform. This platform automates end-to-end health claims, and the abuse & fraud detection capacity is almost 30% or more. Moreover, it enables users to self-learn and develop a system for decision-making, risk assessment, and fraud detection. This growth in the availability of the software is because of increasing healthcare expenditure, which triggers the companies to come up with a product or service to meet the market demand.
The rising incidence of fraudulent activities in the healthcare sector drives the market globally. For example, according to data published by the National Library of Medicine, the fraudulent activities count raised from 30 in 2019 to 52 in the year 2021. The market is highly competitive and consists of several major players. With the rising adoption of healthcare IT solutions and the increasing number of fraud cases, smaller or private players are anticipated to enter the market in the coming years.
Initiatives like collaborations or partnerships with local players, acquisitions, or new product launches by market players contribute to the market growth. For example, in April 2019, HCL Technologies Limited launched the CyberSecurity Fusion Center in Texas, U.S., and expanded its U.S. operations with the CyberSecurity Center.
Scope of The Report
| Report Coverage | Details |
| Market Size in 2021 | USD 1.73 billion |
| Revenue Forecast by 2030 | USD 11.4 billion |
| Growth rate from 2022 to 2030 | CAGR of 23.31% |
| Base Year | 2021 |
| Forecast Period | 2022 to 2030 |
| Segmentation | Solution type, delivery model, application, end-user, region |
| Companies Covered | IBM; Optum, Inc.; Cotiviti, Inc.; DXC Technology; SAS Institute, Inc.; EXL Service Holdings, Inc.; Wipro Limited; Conduent, Inc.; HCL Technologies Limited; OSP Labs |
Solution Type Insights
The descriptive analytics segment held the largest market share of around 40.0% in 2021, owing to its high adoption due to ease of use. It utilizes current as well as historical data for the identification of trends and relationships. This helps in the identification of possible frauds in a better way. It also acts as a base for an effective application of prescriptive and predictive analytics. This further supports the segment’s growth.
The predictive analytics segment is anticipated to witness the fastest growth during the projected period. The most effective way for preventing fraud is by identifying them before the claims are paid. Owing to this, healthcare payers have started adopting predictive analytics solutions. These solutions identify the patterns that are potentially fraudulent, and then develop some rules to flag certain claims.
The prescriptive analytics segment is also expected to witness significant growth, as they also help in evaluating the cost and benefit of a certain solution and help them organize to analyze if they are spending more on trying to catch the fraud, as compared to what they would be losing from the potential fraud.
Delivery Model Insights
The on-premise segment held the highest revenue share of more than 51% in 2021, owing to the ease of access of data being on the site, i.e., hospitals, etc. which has resulted in better management of records as well as monitoring of the data, among other things. Current systems in small organizations are practical, but when scaled up it can be difficult and cumbersome to manage data if the organization is dealing with a large dataset. This can mean large capital investment in the storage and security of data.
The cloud-based segment is estimated to witness the fastest growth of 26.2% during the forecast period, as it has been the emerging delivery mode because it provides a larger space virtually to store data for a multitude of patients. This is cost-effective and is commercially a more viable option for industries. Limitations of this segment include more security concerns regarding loss of data and less privacy.
Application Insights
The insurance claims review segment held the largest market share of over 35% in 2021, due to the rising adoption of health insurance by people, which also results in a growing number of fraudulent claims. The segment is further divided into post-payment review and prepayment review. The prepayment review segment is likely to grow at the fastest CAGR owing to its rising demand from healthcare providers.
The pharmacy billing issue segment is also expected to grow significantly, owing to the rising number of medical billing frauds occurring in the pharmacies. Similarly, the payment integrity segment is also likely to expand at a considerable growth rate. Payment integrity is a tool, which payers use for tightening the administrative side to lower the costs.
End-User Insights
By end-user, public & government agencies dominated with a share of over 41.0% in 2021 in the healthcare fraud analytics market. The key factors contributing to the large share include a higher volume of patients in government hospitals, and the high vulnerability of government agencies to fraudulent activities due to the lack of technologically advanced infrastructure, especially in the developing nations.
The employers' segment is anticipated to grow at the highest CAGR during the projected period, owing to the increasing demand for healthcare fraud analytics by employers for enabling better cost management. The private insurance payers segment is also estimated to witness significant growth, owing to the rising use of fraud analytics solutions for combating the growing monetary losses.
Regional Insights
North America dominated the global market with a share of around 38% in 2021. This is owing to the rising healthcare spending, increasing healthcare IT adoption, and the growing number of fraud cases. According to data published by the National Library of Medicine, fraudulent activities are more commonly seen in the North America region, followed by Europe and Asia Pacific region, in the year 2020. Asia Pacific region is likely to witness the fastest growth rate of around 26.7% during the projected period, owing to the increasing adoption of technologically advanced solutions.
According to National Health Care Anti-Fraud Association (NHCAA), the United States spends over USD 2.27 trillion on health care every year. Of that amount, NHCAA estimates that tens of billions of dollars are lost to health care fraud. Thus, owing to the availability of numerous advanced services and solutions related to healthcare fraud detection, and strategic steps taken by major players present in the country, it is expected to drive the growth of the studied market in the North America region during the projection period.
Key Players
Market Segmentation
Chapter 1. Introduction
1.1.Research Objective
1.2.Scope of the Study
1.3.Definition
Chapter 2. Research Methodology
2.1.Research Approach
2.2.Data Sources
2.3.Assumptions & Limitations
Chapter 3. Executive Summary
3.1.Market Snapshot
Chapter 4. Market Variables and Scope
4.1.Introduction
4.2.Market Classification and Scope
4.3.Industry Value Chain Analysis
4.3.1. Raw Material Procurement Analysis
4.3.2. Sales and Distribution Channel Analysis
4.3.3. Downstream Buyer Analysis
Chapter 5. COVID 19 Impact on Healthcare Fraud Analytics Market
5.1.COVID-19 Landscape: Healthcare Fraud Analytics Industry Impact
5.2.COVID 19 - Impact Assessment for the Industry
5.3.COVID 19 Impact: Global Major Government Policy
5.4.Market Trends and Opportunities in the COVID-19 Landscape
Chapter 6. Market Dynamics Analysis and Trends
6.1.Market Dynamics
6.1.1. Market Drivers
6.1.2. Market Restraints
6.1.3. Market Opportunities
6.2.Porter’s Five Forces Analysis
6.2.1. Bargaining power of suppliers
6.2.2. Bargaining power of buyers
6.2.3. Threat of substitute
6.2.4. Threat of new entrants
6.2.5. Degree of competition
Chapter 7. Competitive Landscape
7.1.1. Company Market Share/Positioning Analysis
7.1.2. Key Strategies Adopted by Players
7.1.3. Vendor Landscape
7.1.3.1. List of Suppliers
7.1.3.2. List of Buyers
Chapter 8. Global Healthcare Fraud Analytics Market, By Solution Type
8.1.Healthcare Fraud Analytics Market, by Solution Type, 2022-2030
8.1.1. Descriptive Analytics
8.1.1.1. Market Revenue and Forecast (2017-2030)
8.1.2. Prescriptive Analytics
8.1.2.1. Market Revenue and Forecast (2017-2030)
8.1.3. Predictive Analytics
8.1.3.1. Market Revenue and Forecast (2017-2030)
Chapter 9. Global Healthcare Fraud Analytics Market, By Delivery Model
9.1.Healthcare Fraud Analytics Market, by Delivery Model, 2022-2030
9.1.1. On-premises
9.1.1.1. Market Revenue and Forecast (2017-2030)
9.1.2. Cloud-based
9.1.2.1. Market Revenue and Forecast (2017-2030)
Chapter 10.Global Healthcare Fraud Analytics Market, By Application Type
10.1.Healthcare Fraud Analytics Market, by Application Type, 2022-2030
10.1.1.Insurance Claim Review
10.1.1.1.Market Revenue and Forecast (2017-2030)
10.1.2.Pharmacy billing Issue
10.1.2.1.Market Revenue and Forecast (2017-2030)
10.1.3.Payment Integrity
10.1.3.1.Market Revenue and Forecast (2017-2030)
10.1.4.Others
10.1.4.1.Market Revenue and Forecast (2017-2030)
Chapter 11.Global Healthcare Fraud Analytics Market, By End User
11.1.Healthcare Fraud Analytics Market, by End User, 2022-2030
11.1.1.Public & Government Agencies
11.1.1.1.Market Revenue and Forecast (2017-2030)
11.1.2.Private Insurance Payers
11.1.2.1.Market Revenue and Forecast (2017-2030)
11.1.3.Third-party Service Providers
11.1.3.1.Market Revenue and Forecast (2017-2030)
11.1.4.Employers
11.1.4.1.Market Revenue and Forecast (2017-2030)
Chapter 12.Global Healthcare Fraud Analytics Market, Regional Estimates and Trend Forecast
12.1.North America
12.1.1.Market Revenue and Forecast, by Solution Type (2017-2030)
12.1.2.Market Revenue and Forecast, by Delivery Model (2017-2030)
12.1.3.Market Revenue and Forecast, by Application Type (2017-2030)
12.1.4.Market Revenue and Forecast, by End User (2017-2030)
12.1.5.U.S.
12.1.5.1.Market Revenue and Forecast, by Solution Type (2017-2030)
12.1.5.2.Market Revenue and Forecast, by Delivery Model (2017-2030)
12.1.5.3.Market Revenue and Forecast, by Application Type (2017-2030)
12.1.5.4.Market Revenue and Forecast, by End User (2017-2030)
12.1.6.Rest of North America
12.1.6.1.Market Revenue and Forecast, by Solution Type (2017-2030)
12.1.6.2.Market Revenue and Forecast, by Delivery Model (2017-2030)
12.1.6.3.Market Revenue and Forecast, by Application Type (2017-2030)
12.1.6.4.Market Revenue and Forecast, by End User (2017-2030)
12.2.Europe
12.2.1.Market Revenue and Forecast, by Solution Type (2017-2030)
12.2.2.Market Revenue and Forecast, by Delivery Model (2017-2030)
12.2.3.Market Revenue and Forecast, by Application Type (2017-2030)
12.2.4.Market Revenue and Forecast, by End User (2017-2030)
12.2.5.UK
12.2.5.1.Market Revenue and Forecast, by Solution Type (2017-2030)
12.2.5.2.Market Revenue and Forecast, by Delivery Model (2017-2030)
12.2.5.3.Market Revenue and Forecast, by Application Type (2017-2030)
12.2.5.4.Market Revenue and Forecast, by End User (2017-2030)
12.2.6.Germany
12.2.6.1.Market Revenue and Forecast, by Solution Type (2017-2030)
12.2.6.2.Market Revenue and Forecast, by Delivery Model (2017-2030)
12.2.6.3.Market Revenue and Forecast, by Application Type (2017-2030)
12.2.6.4.Market Revenue and Forecast, by End User (2017-2030)
12.2.7.France
12.2.7.1.Market Revenue and Forecast, by Solution Type (2017-2030)
12.2.7.2.Market Revenue and Forecast, by Delivery Model (2017-2030)
12.2.7.3.Market Revenue and Forecast, by Application Type (2017-2030)
12.2.7.4.Market Revenue and Forecast, by End User (2017-2030)
12.2.8.Rest of Europe
12.2.8.1.Market Revenue and Forecast, by Solution Type (2017-2030)
12.2.8.2.Market Revenue and Forecast, by Delivery Model (2017-2030)
12.2.8.3.Market Revenue and Forecast, by Application Type (2017-2030)
12.2.8.4.Market Revenue and Forecast, by End User (2017-2030)
12.3.APAC
12.3.1.Market Revenue and Forecast, by Solution Type (2017-2030)
12.3.2.Market Revenue and Forecast, by Delivery Model (2017-2030)
12.3.3.Market Revenue and Forecast, by Application Type (2017-2030)
12.3.4.Market Revenue and Forecast, by End User (2017-2030)
12.3.5.India
12.3.5.1.Market Revenue and Forecast, by Solution Type (2017-2030)
12.3.5.2.Market Revenue and Forecast, by Delivery Model (2017-2030)
12.3.5.3.Market Revenue and Forecast, by Application Type (2017-2030)
12.3.5.4.Market Revenue and Forecast, by End User (2017-2030)
12.3.6.China
12.3.6.1.Market Revenue and Forecast, by Solution Type (2017-2030)
12.3.6.2.Market Revenue and Forecast, by Delivery Model (2017-2030)
12.3.6.3.Market Revenue and Forecast, by Application Type (2017-2030)
12.3.6.4.Market Revenue and Forecast, by End User (2017-2030)
12.3.7.Japan
12.3.7.1.Market Revenue and Forecast, by Solution Type (2017-2030)
12.3.7.2.Market Revenue and Forecast, by Delivery Model (2017-2030)
12.3.7.3.Market Revenue and Forecast, by Application Type (2017-2030)
12.3.7.4.Market Revenue and Forecast, by End User (2017-2030)
12.3.8.Rest of APAC
12.3.8.1.Market Revenue and Forecast, by Solution Type (2017-2030)
12.3.8.2.Market Revenue and Forecast, by Delivery Model (2017-2030)
12.3.8.3.Market Revenue and Forecast, by Application Type (2017-2030)
12.3.8.4.Market Revenue and Forecast, by End User (2017-2030)
12.4.MEA
12.4.1.Market Revenue and Forecast, by Solution Type (2017-2030)
12.4.2.Market Revenue and Forecast, by Delivery Model (2017-2030)
12.4.3.Market Revenue and Forecast, by Application Type (2017-2030)
12.4.4.Market Revenue and Forecast, by End User (2017-2030)
12.4.5.GCC
12.4.5.1.Market Revenue and Forecast, by Solution Type (2017-2030)
12.4.5.2.Market Revenue and Forecast, by Delivery Model (2017-2030)
12.4.5.3.Market Revenue and Forecast, by Application Type (2017-2030)
12.4.5.4.Market Revenue and Forecast, by End User (2017-2030)
12.4.6.North Africa
12.4.6.1.Market Revenue and Forecast, by Solution Type (2017-2030)
12.4.6.2.Market Revenue and Forecast, by Delivery Model (2017-2030)
12.4.6.3.Market Revenue and Forecast, by Application Type (2017-2030)
12.4.6.4.Market Revenue and Forecast, by End User (2017-2030)
12.4.7.South Africa
12.4.7.1.Market Revenue and Forecast, by Solution Type (2017-2030)
12.4.7.2.Market Revenue and Forecast, by Delivery Model (2017-2030)
12.4.7.3.Market Revenue and Forecast, by Application Type (2017-2030)
12.4.7.4.Market Revenue and Forecast, by End User (2017-2030)
12.4.8.Rest of MEA
12.4.8.1.Market Revenue and Forecast, by Solution Type (2017-2030)
12.4.8.2.Market Revenue and Forecast, by Delivery Model (2017-2030)
12.4.8.3.Market Revenue and Forecast, by Application Type (2017-2030)
12.4.8.4.Market Revenue and Forecast, by End User (2017-2030)
12.5.Latin America
12.5.1.Market Revenue and Forecast, by Solution Type (2017-2030)
12.5.2.Market Revenue and Forecast, by Delivery Model (2017-2030)
12.5.3.Market Revenue and Forecast, by Application Type (2017-2030)
12.5.4.Market Revenue and Forecast, by End User (2017-2030)
12.5.5.Brazil
12.5.5.1.Market Revenue and Forecast, by Solution Type (2017-2030)
12.5.5.2.Market Revenue and Forecast, by Delivery Model (2017-2030)
12.5.5.3.Market Revenue and Forecast, by Application Type (2017-2030)
12.5.5.4.Market Revenue and Forecast, by End User (2017-2030)
12.5.6.Rest of LATAM
12.5.6.1.Market Revenue and Forecast, by Solution Type (2017-2030)
12.5.6.2.Market Revenue and Forecast, by Delivery Model (2017-2030)
12.5.6.3.Market Revenue and Forecast, by Application Type (2017-2030)
12.5.6.4.Market Revenue and Forecast, by End User (2017-2030)
Chapter 13.Company Profiles
13.1.IBM
13.1.1.Company Overview
13.1.2.Product Offerings
13.1.3.Financial Performance
13.1.4.Recent Initiatives
13.2.Optum, Inc.
13.2.1.Company Overview
13.2.2.Product Offerings
13.2.3.Financial Performance
13.2.4.Recent Initiatives
13.3.Cotiviti, Inc
13.3.1.Company Overview
13.3.2.Product Offerings
13.3.3.Financial Performance
13.3.4.Recent Initiatives
13.4.DXC Technology
13.4.1.Company Overview
13.4.2.Product Offerings
13.4.3.Financial Performance
13.4.4.Recent Initiatives
13.5.SAS Institute, Inc.
13.5.1.Company Overview
13.5.2.Product Offerings
13.5.3.Financial Performance
13.5.4.Recent Initiatives
13.6.EXL Service Holdings, Inc.
13.6.1.Company Overview
13.6.2.Product Offerings
13.6.3.Financial Performance
13.6.4.Recent Initiatives
13.7.Wipro Limited
13.7.1.Company Overview
13.7.2.Product Offerings
13.7.3.Financial Performance
13.7.4.Recent Initiatives
13.8.Conduent, Inc
13.8.1.Company Overview
13.8.2.Product Offerings
13.8.3.Financial Performance
13.8.4.Recent Initiatives
13.9.HCL Technologies Limited
13.9.1.Company Overview
13.9.2.Product Offerings
13.9.3.Financial Performance
13.9.4.Recent Initiatives
13.10.OSP Labs
13.10.1. Company Overview
13.10.2. Product Offerings
13.10.3. Financial Performance
13.10.4. Recent Initiatives
Chapter 14.Research Methodology
14.1.Primary Research
14.2.Secondary Research
14.3.Assumptions
Chapter 15.Appendix
15.1.About Us
15.2.Glossary of Terms
 Cross-segment Market Size and Analysis for
Mentioned Segments
Cross-segment Market Size and Analysis for
Mentioned Segments
 Additional Company Profiles (Upto 5 With No Cost)
Additional Company Profiles (Upto 5 With No Cost)
 Additional Countries (Apart From Mentioned Countries)
Additional Countries (Apart From Mentioned Countries)
 Country/Region-specific Report
Country/Region-specific Report
 Go To Market Strategy
Go To Market Strategy
 Region Specific Market Dynamics
Region Specific Market Dynamics Region Level Market Share
Region Level Market Share Import Export Analysis
Import Export Analysis Production Analysis
Production Analysis Others
Others